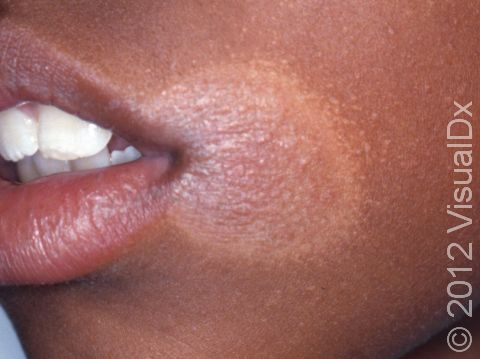
Pityriasis Alba
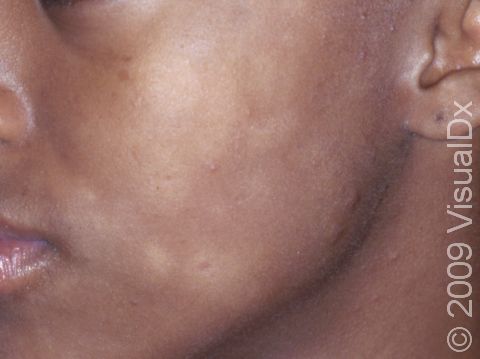
Pityriasis alba is a common noncancerous (benign) skin condition affecting children. It appears as light-colored patches, especially on the cheeks.
Although the condition typically lasts 1 year or more without treatment, pityriasis alba usually resolves after puberty or by the time the child reaches adulthood.
The exact cause of pityriasis alba is unknown, though triggers may include:
- Heat
- Humidity
- Heavily scented detergents or soaps
- Abrasive clothing
- Smoke
- Stress
Who's At Risk?
Pityriasis alba occurs in children of all races and of both sexes. It is most common in children aged 3–16 years.
Children at higher risk for pityriasis alba include those with:
- Asthma
- Hayfever (allergic rhinitis)
- Eczema (atopic dermatitis)
- Dry skin (xerosis)
Signs & Symptoms
The most common locations for pityriasis alba include:
- Cheeks, around the mouth, chin
- Forehead
- Neck
- Shoulders, upper chest, and upper arms
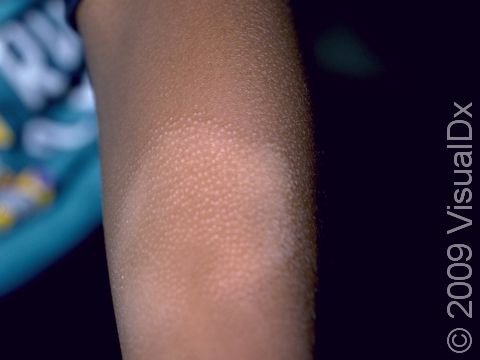
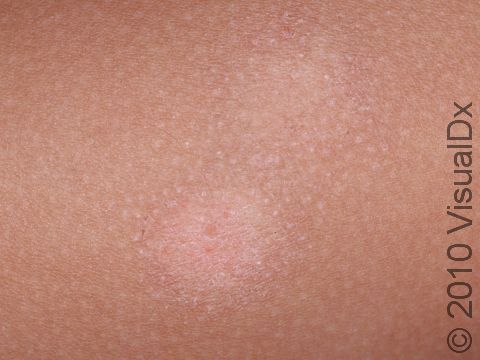
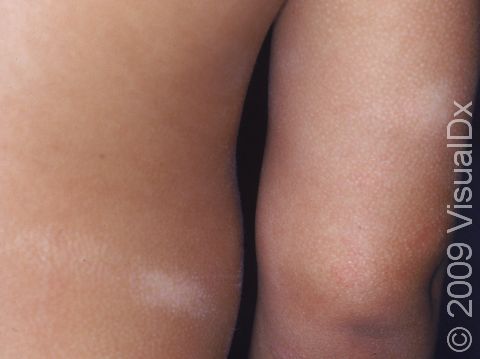
Pityriasis alba appears as several (2–20) light-colored (hypopigmented) patches ranging in size from 1–4 cm. The patches may have slight and subtle surface patches (scale). Occasionally, the condition begins as mildly itchy, pink patches that develop into lightened patches of skin.
People often think that pityriasis alba gets worse in the summer, but it just becomes more obvious as the normal, surrounding skin becomes darker with sun exposure.
Self-Care Guidelines
If you suspect that your child has pityriasis alba, the most important self-care measure is to keep the skin well moisturized. Try the following:
- Use non-soap cleansers or moisturizing soaps.
- Apply moisturizers such as petroleum jelly (Vaseline®) or fragrance-free ointments and creams.
- Avoid sun exposure and wear sunscreen.
- Apply over-the-counter hydrocortisone cream sparingly for 3–7 days.
Treatments
To make sure that there is no yeast or fungus present, your physician may wish to scrape some of the scales onto a slide and examine them under a microscope. This procedure, called a KOH (potassium hydroxide) preparation, allows the doctor to look for tell-tale signs of yeast infection. Pityriasis alba is not caused by an infection with yeast or fungus. Therefore, the KOH preparation should be negative.
Since pityriasis alba is benign and does not usually spread or last long, no treatment may be necessary. The physician will recommend many of the self-care measures listed above. In very severe widespread infections with pityriasis alba, the doctor may recommend:
- Prescription-strength corticosteroid (cortisone) cream
- Ultraviolet light therapy
Visit Urgency
Call your child’s doctor for evaluation if the condition does not improve with self-care measures, if it seems to be getting worse, or if it spreads to other areas.
Trusted Links
References
Bolognia, Jean L., ed. Dermatology, pp.223-224, 965. New York: Mosby, 2003.
Freedberg, Irwin M., ed. Fitzpatrick’s Dermatology in General Medicine. 6th ed. pp.837-838, 858. New York: McGraw-Hill, 2003.
Last modified on October 10th, 2022 at 8:29 pm
Not sure what to look for?
Try our new Rash and Skin Condition Finder